What is shoulder degeneration or shoulder osteoarthritis?
Shoulder osteoarthritis (OA), is a degenerative joint disease generally described as the gradual degeneration of the cartilage and other tissues in the glenohumeral joint.
Even non-weight bearing joints such as the shoulder joint are prone to wear and tear and injury. The pain and stiffness caused by shoulder degeneration can affect arm movement making it difficult to hit a golf ball, retrieve items from an overhead shelf, or even brush one's teeth.
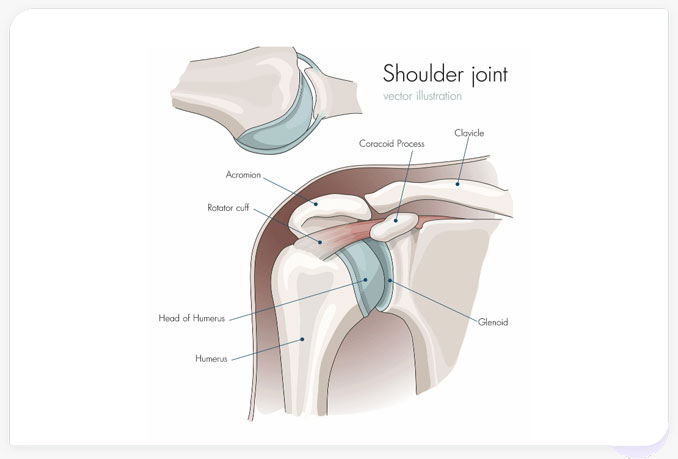
Glenohumeral degenerative joint disease involves damage to the articular cartilage and other tissues associated with the glenohumeral joint. Articular cartilage lines the surface of the humeral head and glenoid in the joint (see Figure 1) enabling the bones to glide against each other acting as a buffer between abutting bones. As this normally strong, slippery cartilage wears, friction within the joint increases causing stiffness and pain.
Figure 1. The shoulder joint (glenohumeral joint) is a ball and socket joint between the scapula (shoulder blade) and the humerus (upper arm bone between the shoulder and elbow). The glenoid is the portion of the scapula that forms the shoulder joint with the humerus. Being one of the most mobile joints in the human body comes at the cost of joint stability.
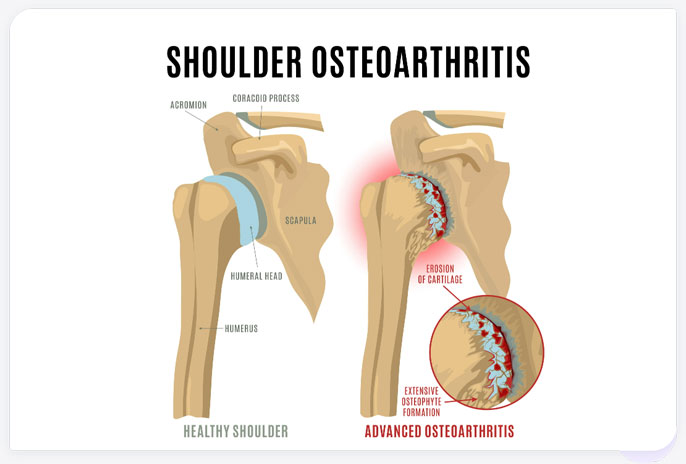
The humerus and glenoid may also produce excess cells that form osteophytes or bone spurs in response to the damaged articular cartilage (see Figure 2). Bone spurs may result in further bone-on-bone friction negatively impacting the shoulder's range of motion and causing pain.
Figure 2. Stages of osteoarthritis (OA) of the shoulder joint. In a healthy joint the articular cartilage is smooth and free of osteophytes or bone spurs. As OA progresses into moderate and advanced stages, the articular cartilage erodes and osteophyte formation increases. This degeneration of the joint causes significant pain, stiffness, and loss of function.
Signs & Symptoms

Pain is the most obvious symptom of shoulder and other forms of osteoarthritis. Other symptoms include:
- Shoulder pain. Moderate to severe disease may cause a chronic dull aching pain or flare-ups of pain that can interfere with sleep. Pain usually occurs at the back of the shoulder.
- Stiffness or loss of motion. A decreased range of motion is observed making bathing, getting dressed, and other daily activities challenging. Inactivity can make stiffness even worse.
- Catching. When the shoulder "catches" smooth movements are involuntarily interrupted.
- Crepitus. Crunching or popping sounds that occur when rotating the shoulder is a sign that the protective articular cartilage has worn away causing friction in the shoulder joint.
- Weakness and muscle atrophy. Muscle degeneration occurs when weight bearing movements (e.g., lifting objects) are avoided because they are painful to perform.
- Swelling. The soft tissues surrounding the shoulder joint can become irritated and swell. Swelling is usually less severe than in knee or hand arthritis.
Shoulder arthritis is largely due to years of wear and tear that damages cartilage in the joint.
Other causes and risk factors include:- Age. Beside increased wear and tear over time, aging leads to morphological and biochemical changes in the cells of joint tissues further increasing the susceptibility of older adults to OA.
- Sex. Women are more likely to develop glenohumeral joint osteoarthritis, this may be due to age-related nutritional deficiencies and hormonal changes.
- Obesity. Being overweight places excess burden on the body's joints and may increase the pace of cartilage degeneration.
- Repeated joint stress. Repetitive activities lead to more wear and tear especially in occupations that require lifting objects overhead or in high-impact activities (tennis, golf, hammering, jackhammering etc.).
- Genetics. There is a higher risk of developing OA if it runs in the family. Congenital defects leading to poor bone alignment also increase the risk of dislocations and OA.
- Bone deformities. Misaligned joints due to abnormal bone structure increase the stress at the joint and may contribute to OA and glenohumeral joint pain.
- Metabolic diseases. Changes the mineral content and health of the tissues and bone in the shoulder joint can lead to increased risk for OA.
- Previous injury to the shoulder. Having a history of shoulder dislocation, broken bones, or shoulder surgeries increase the risk of developing OA due to the weakening of the glenohumeral joint ligaments and other joint tissues.

Shoulder OA is diagnosed by our Specialists using a multipronged approach.
- Medical History: Our doctors will ask you about the nature of your shoulder pain (e.g., when and under what conditions you experience shoulder pain). They will ask about prior surgeries, accidents, and trauma to the shoulder.
- Physical Exam: The doctor will examine the range of motion of the shoulder and assess the location and severity of your shoulder pain.
- Imaging with X-Rays, MRI, or ultrasound: X-rays are used to confirm shoulder pain due to osteoarthritis. A magnetic resonance imaging (MRI) scan or ultrasound may be used to determine if there is damage to surrounding joint tissues.
Treatment Options
The StemX clinic offers a range of customized Regenerative Medicine treatment solutions for shoulder OA.
The StemX Approach
StemX is California's leading provider of holistic and regenerative medicine services. Our experts don't just offer popular treatments, but customized medical solutions based on individual needs.
Located in Solana Beach, California, the StemX clinic is composed of a team of expert doctors with years of experience administering regenerative medicine treatments for joint disease. Our team has:
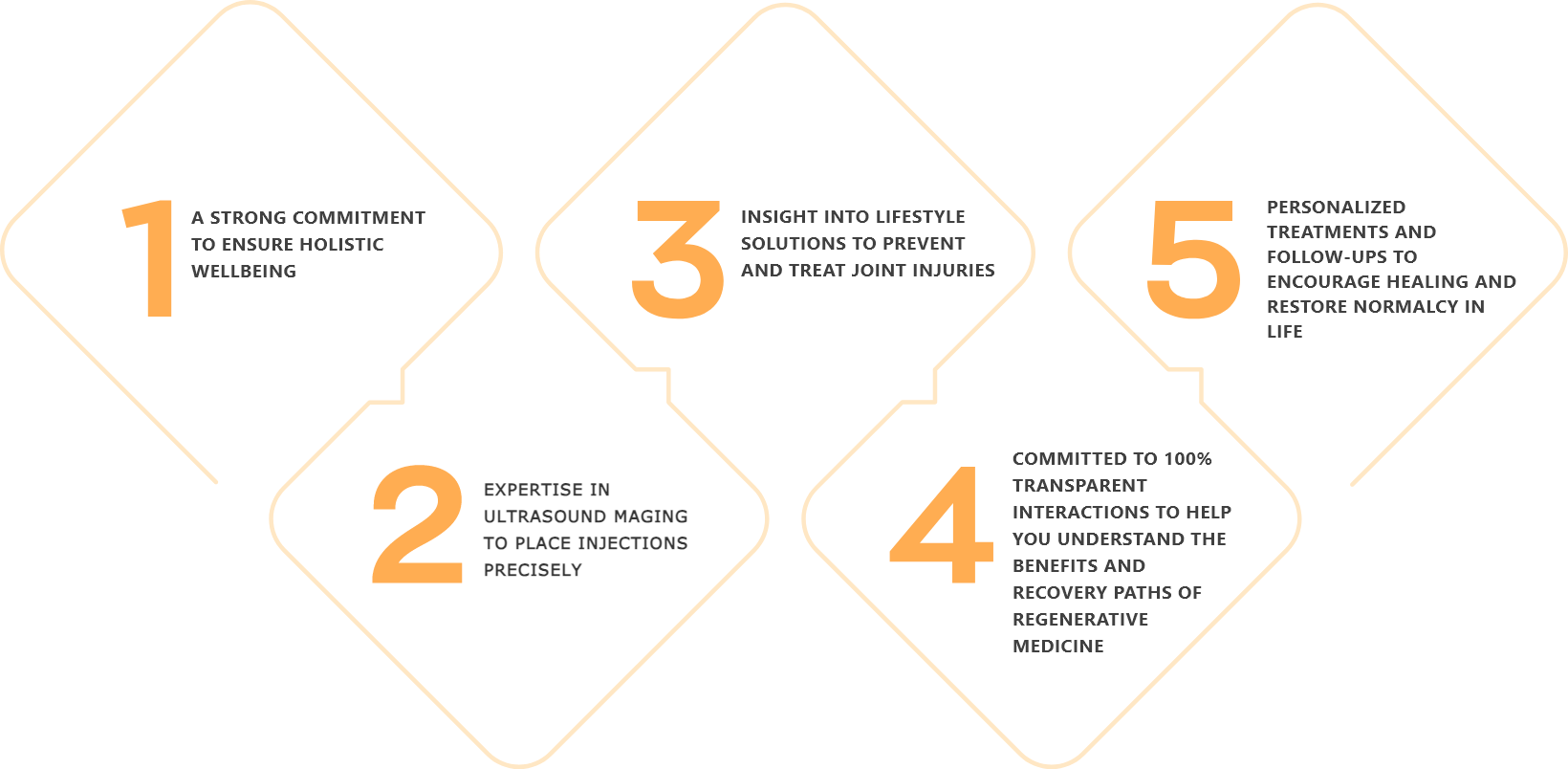





How To Get Started
Treatment Procedure
While each treatment may be customized, you can expect your experience to be similar to the following:




All procedures are conducted in our Solana Beach, California clinic. 124 Lomas Santa Fe Dr #206, Solana Beach, CA 92075.
Frequently Asked Questions
Shoulder degeneration (or osteoarthritis) refers to the loss of the cartilage in the glenohumeral joint and damage to surrounding muscles, tendons, and tissues.
Several non-surgical treatment options exist. NSAIDs, steroids, or natural regenerative medicine treatments are usually effective without resorting to surgery.
If you are very active, your shoulders are prone to degeneration. Also, with age comes wear and tear on the joint. Traumatic injury may also cause shoulder joint degeneration and osteoarthritis.
Glenohumeral joint injections with steroids can alleviate moderate to severe pain but may have side effects. StemX's regenerative treatments can provide relief naturally with no side effects.
Unfortunately, osteoarthritis is a degenerative, progressive disease that requires treatment once the damage is done. Steps can be taken to prevent the disease from worsening, however.
Regenerative Medicine treatments require 6-12 weeks for full efficacy, this is dependent on the extent of damage and age of patient. Shoulder replacement surgery requires 12 weeks or more to recover.
Moderate to severe disease may cause a chronic dull aching pain or flare-ups of pain that can interfere with sleep. Pain usually occurs at the back of the shoulder.
Your doctor and physical therapist should be consulted before starting an exercise regimen that can help strengthen the shoulder muscles and tendons to prevent further injuring the joint.
Resting the shoulder, modifying activities that cause wear and tear together with regenerative medicine therapies can work together to quickly heal your joint.
No, there are four different joints in the shoulder. The glenohumeral joint is between the humerus and the scapula. The acromioclavicular joint is between the acromion and the collar bone.
Regenerative medicine treatments can last from months to years depending on the patient's activity levels and disease severity. Athletes may need repeated treatments, for example.
Regenerative medicine treatments cause minimal discomfort and consist of a simple injection into the joint space. The joint may be sore a few days after the injection.



