Regenerative Medicine
Alternative to Knee Replacement Surgery
Heal Naturally with Regenerative Therapies
What Is Osteoarthritis
Of The Knee?
Osteoarthritis (OA) of the knee is a progressive condition that causes aching pain, stiffness, and loss of mobility in the knee. Because OA is a degenerative disease due to wear and tear of the joint cartilage, symptoms gradually worsen.
Musculoskeletal joint conditions are extremely prevalent in the US. Osteoarthritis is the most common of the dozens of forms of arthritis. OA can affect any joint but is extremely prevalent in the knees.
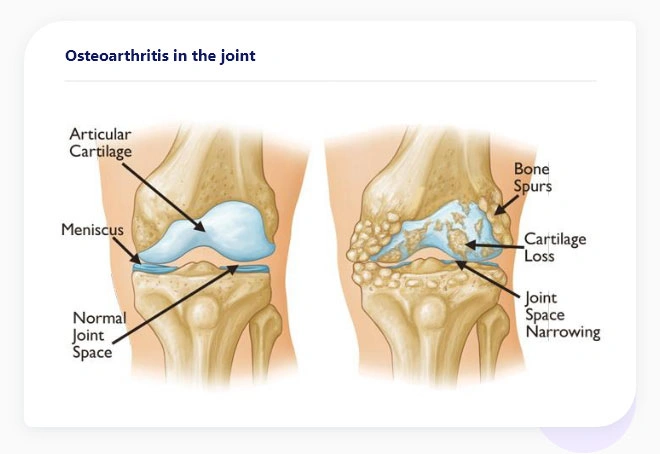
The knee being the largest joint in the body is also one of the strongest (See Figure 1). It’s composed of three bones: the bottom part of the thighbone (the femur); the top part of the shinbone (tibia); and a large, round bone that covers and protects the joint (the patella or kneecap). The ends of these bones are lined in a smooth protective material called articular cartilage that acts like a shock absorber and helps the bones to move easily past each other while the body is in motion.
Figure 1. Depiction of a normal knee joint. Note the amount of joint space and smooth surface of the articular cartilage in the normal knee. (right) Depiction of osteoarthritic knee with articular cartilage loss, bone spurs, and narrowing of the joint space.
Causes, Signs And Symptoms
What causes knee osteoarthritis?The ultimate cause of knee pain and other osteoarthritis symptoms is often bone-on-bone friction as the cartilage begins to erode (See Figure 2). Over time, cartilage may wear away completely, leaving the joint vulnerable to permanent damage.
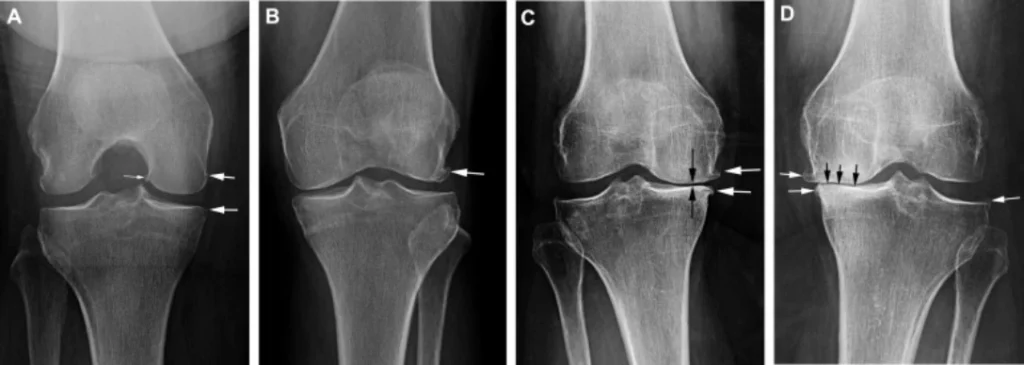
Figure 2. Phases of Osteoarthritic Knee Degeneration (knee osteoarthritis pictures).
(A) Black arrows point to the joint space between the femur and tibia in a healthy knee.
(B) Osteophyte formation is denoted by the white arrow marking the beginning of clinically graded osteoarthritis.
(C) Joint space gradually lessens with disease progression ultimately leading to D) a near complete loss of joint space in severe osteoarthritis, denoted by black arrows.

What are the symptoms of knee osteoarthritis?
Pain from Knee OA may be experienced as a dull chronic pain that worsens after activity. In severe cases, the pain may become debilitating, limiting mobility, and preventing normal daily activities.
Patients with arthritis in the knee may experience one or more of the following symptoms:
What are the risk factors for developing knee osteoarthritis?
Age is the biggest risk factor for OA which is most common in adults 50 years and older, although trauma to the joint due to accidents or sports injuries are also significant risk factors across age groups.
The following are the major risk factors for knee osteoarthritis:

How is knee osteoarthritis diagnosed?
Patients are seen in our California-based clinic where our specialists will base their diagnosis of knee osteoarthritis using a multipronged approach:
Treatment Options
How are knee meniscus tears treated?
The StemX clinic offers a range of customized Regenerative Medicine treatments to treat orthopedic injuries.
Wharton’s Jelly
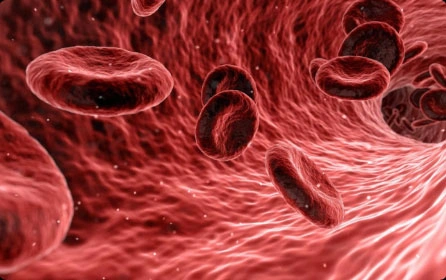
PRP
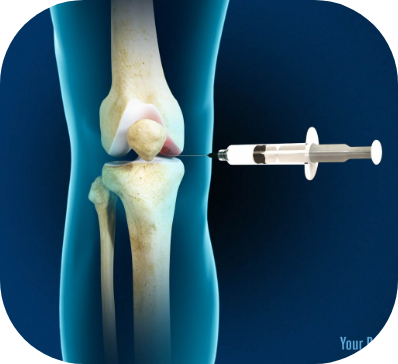
Hyaluronic Acid/
Prolotherapy
The StemX Approach
StemX is California’s leading provider of holistic and regenerative medicine services. Our experts don’t just offer popular treatments, but customized medical solutions based on individual needs.
Located in Solana Beach, California, the StemX clinic is composed of a team of expert doctors with years of experience administering regenerative medicine treatments for joint disease. Our team has:
How To Get Started
Consultation:
Our California-based clinic intake team will match you to the appropriate provider with the expertise to treat your injury and schedule an exam.
Initial Exam:
Your doctor will take your medical history and facts surrounding your injury/complaint, conduct a physical exam, and order imaging tests (X-rays, MRI’s, etc.).
Treatment determination:
Use this space to add a short description. It gives enough info to earn a click.
Mark your calendar:
A date will be set for your procedure, and you will be given instructions on how to prepare for your appointment.
Treatment Procedure
While each treatment may be customized, you can expect your experience to be similar to the following:



